Clinic Appointment in July 2021: Abnormal Blood Results and Weight Gain
In July 2021, my fasting sugar level was borderline, some liver enzymes were slightly high, and I had put on 3.5 kg in weight.
On July 6, 2021, I had some “routine” blood investigations – a complete blood count, fasting blood sugar, lipid profile, renal function test, liver function test, and urinalysis. I had a scheduled gastroenterology appointment on the same day.
I had no symptoms around that time and was feeling fine.
So, when I learned about some abnormalities in the blood tests, I was gobsmacked. They were not abnormal. I just wasn’t expecting anything other than figures within the normal range.
Borderline Fasting Blood Sugar
My fasting blood sugar level was 5.6 mmol/L or 100 mg/dL. The laboratory’s reference ranges were:
| Blood Sugar Classification | Blood Sugar Level (mmol/L) |
|---|---|
| Normal | <5.6 |
| Prediabetes | 5.6–6.9 |
| Diabetes | ≥7.0 |
My previous fasting blood sugar test was on April 17, 2020. My fasting blood sugar was 5.1 mmol/L on that day, i.e., normal.
Liver Function Test
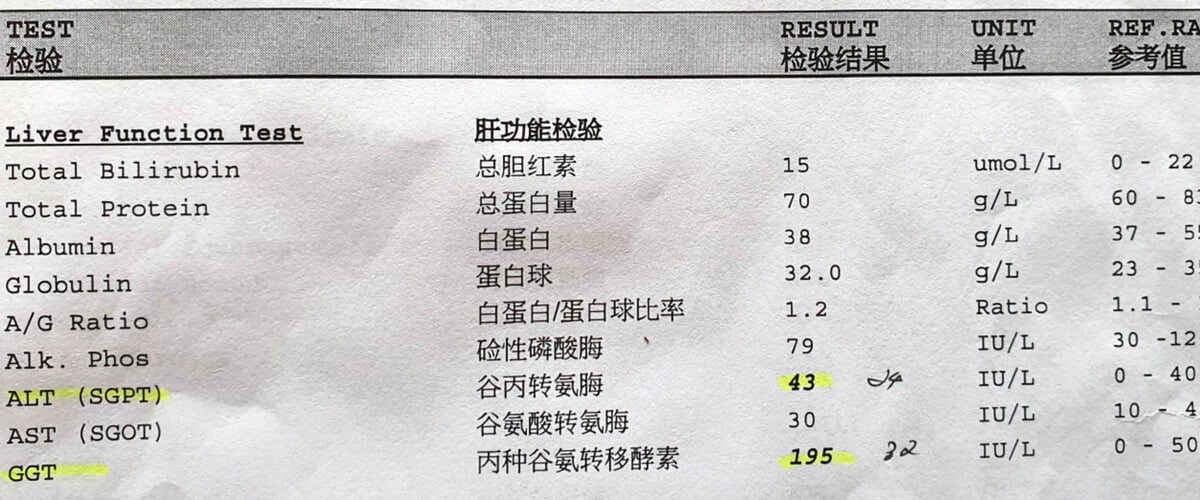
The liver function test showed an elevated ALT and raised GGT.
| Jul 6, 2021 | Apr 17, 2020 | Reference Range | |
|---|---|---|---|
| ALT | 43 | 24 | 0–40 IU/L |
| GGT | 195 | 32 | 0–50 IU/L |
The other biochemical parameters on the liver function test were normal.
My complete blood count, ESR, and CRP were within normal limits. So were my lipid profile and urinalysis. Other than a mildly raised uric acid level (440 µmol/L; reference range: 142–416), my renal function test was also normal.
Weight Gain
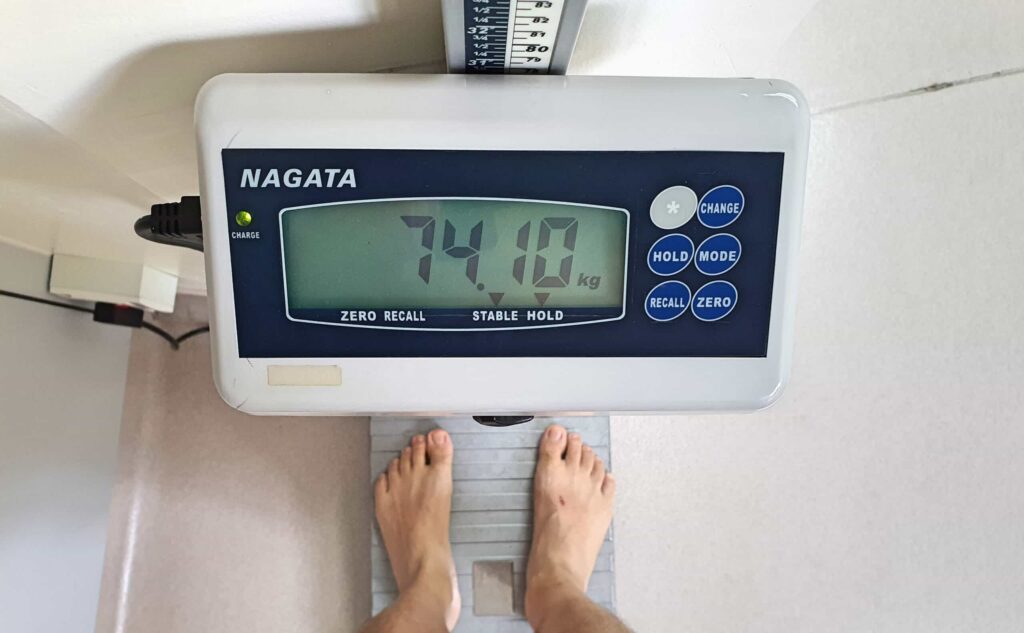
Other than the raised fasting blood sugar, ALT, and GGT, there was one more surprise for me at the hospital: weight gain of 3.5 kg, or nearly 5% of my body weight (!), between January 2021 and July 6, 2021 (6 months).
My gastroenterologist hypothesized that fatty liver caused the raised liver enzymes, possibly because of excess carbohydrates in my diet.
My weight gain would support his hypothesis. He believed the weight gain was mainly more abdominal adipose tissue despite my repeated assertions I had been exercising a lot, and my Strava record was superb.
Putting on weight came out of left field. I had not been monitoring my weight at home – I prefer to only use the industrial-grade digital weight scale at the hospital for validity. Besides, my clothes didn’t feel any tighter, and I didn’t notice any significant change in my facial features, e.g., my cheeks didn’t look any rounder.
Admittedly, the borderline fasting sugar level seemed to suggest some loss of insulin sensitivity. Thanks to my weight gain, it was hard to discount that I had moved closer to being classified as abdominally obese. Abdominal obesity is a risk factor for insulin resistance.
Ulcerative Colitis: Did I Have a Relapse in January 2021?
At the same clinic appointment, my gastroenterologist expressed his reservation about my self-diagnosis of a relapse of my ulcerative colitis in January 2021. According to him, if it were a relapse, I would have experienced bloody diarrhea – I did not notice any blood on my stools. Nevertheless, since I had increased my dose of Salofalk back to 1 gram t.d.s, he was reluctant to lower the dose again.
On July 6, 2021, my C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) – inflammatory markers of disease activity – were normal.
Conclusion
To my mind, I had a few medical problems:
I shall address each of these problems in separate blog posts.