Borderline Blood Glucose Level
My fasting blood glucose level was 5.6 mmol/L, or 100 mg/dL, on July 6, 2021, and October 5, 2021. This level is at the American Diabetes Association’s lower limit for diagnosing impaired fasting glucose.
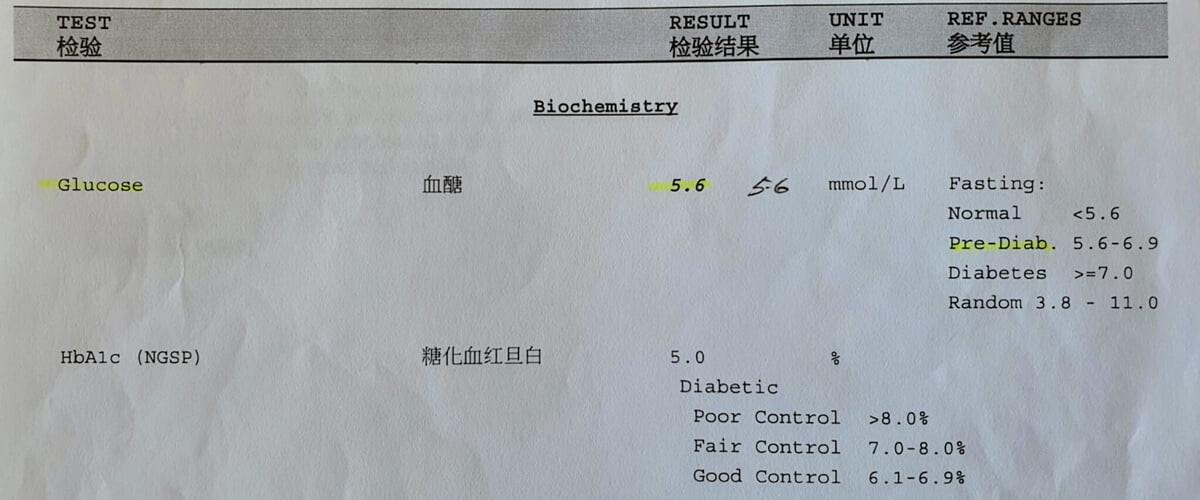
On July 6, 2021, my fasting blood sugar level was 5.6 mmol/L, or 100 mg/dL.
The laboratory reference ranges were:
| Blood Sugar Classification | Blood Sugar Level (mmol/L) |
|---|---|
| Normal | <5.6 |
| Prediabetes | 5.6–6.9 |
| Diabetes | ≥7.0 |
My previous fasting blood sugar level tested on April 17, 2020, i.e., more than a year earlier, was normal at 5.1 mmol/L, or 91.8 mg/dL.
On July 6, 2021, I brushed off the borderline fasting blood sugar as some aberration.
On my next visit to my gastroenterologist on October 5, 2021, a repeat fasting blood sugar test yielded the same result as the July 6 reading – 5.6 mmol/L.
The result was both perplexing and disappointing. I had done all I could to lower my blood sugar levels. I had done the following.
- Regular exercise. Throughout the three months between the clinic visits, I had maintained my long-standing exercise regimen. My Strava records show I had either run or rowed, at moderate intensity, at an average of 26.3 hours per month or 6.6 hours per week. My Strava records don’t show my work to strengthen my core.
- Diet control and modification. I had optimized my daily diet to manage my irritable bowel syndrome (IBS), not my blood sugar. However, my diet was lean, and I couldn’t see how to lower my carbohydrate intake safely. I kept my consumption of complex carbohydrates (mainly steamed brown rice) the same while being careful about the amount of simple sugars, e.g., fruits, table sugar (in my coffee and tea), and Coca-Cola, in my diet. While I didn’t reduce my intake of simple carbohydrates, I attempted to avoid increasing my intake of simple carbohydrates. Other changes were:
- Consuming more animal protein like chicken or pork while watching the concomitant fat intake. Excessive fat consumption precipitates my irritable bowel syndrome (IBS) symptoms, and fatty/oily foods rarely suit my palate.
- A more restrictive form of intermittent fasting. Given my weight gain and the possibility of fatty liver, I thought it was prudent to lose body fat. So, besides my regular exercise and already-calorie-limited diet, I extended my daily fast from around 15 hours to 16 or 17 hours.
- Weight loss. On October 5, 2021, my weight was 67.8 kg – a reduction of 6.3 kg, or 8.5% of my previous total body weight (74.1 kg on July 6, 2021). Most of the weight loss was because of a reduction in fat mass instead of muscle mass. My running and rowing performance had not deteriorated during the 3-month interval between clinic appointments. Because of the weight loss, my running and rowing power-to-weight ratios, which I am far more concerned about than body weight, body composition, or body fat percentage, have even improved. I refrained from cycling because I was due to have a repeat prostate-specific antigen (PSA) test on October 5, 2021, and I wanted nothing to affect that test result. I have previously recounted how cycling had affected my prostate and PSA in Q2 2020.
Over three months, I had continued regular moderate-intensity aerobic exercise (running and rowing), adjusted my diet to lower my blood sugar levels, and lost a significant amount of fat mass. From my point of view, I had done everything I could sans drugs to lower my fasting blood sugar level by October 5, 2021.
But there was no change in my fasting blood sugar – 5.6 mmol/L. This level is at the bottom end of the range for prediabetes. If it were only 0.1 mmol/L less, the level would be normal.
My HbA1c on October 5, 2021, at 5.0%, was well within the normal range (<6.1%).
I did not undergo an oral glucose tolerance test (OGTT).
The parameters of my lipid profile test – total cholesterol, triglycerides, HDL and LDL, total cholesterol to HDL ratio – on July 6, 2021, were all within the laboratory reference ranges for normal.
Risk Factors
I have three risk factors for prediabetes:
- I am over the age of 45
- My father has Type 2 diabetes
- I am of Southeast Asia decent
My lifestyle is healthier than most people’s by a fair margin.
My waist measures 31 inches (or 78.7 cm).
My blood pressure is usually below 140/90 mmHg. My blood lipid profile is normal.
The only medication I take regularly is mesalazine.
I am a lifetime non-smoker.
Symptoms and Signs
Persons with prediabetes usually have no symptoms. I experienced fatigue, but I attributed it to irritable bowel syndrome. I did not experience any other symptoms suggesting diabetes, such as polydipsia, polyphagia, weight loss before July 2021, or urinary frequency.
I looked for but did not find any skin changes that might have been due to acanthosis nigricans. I didn’t notice any skin tags. In the months preceding my July 2021 clinic appointment, my vision had not altered.
Diagnosis of Prediabetes
Fasting Glucose
The American Diabetes Association’s lower cut-off value for impaired fasting glucose (100 mg/dL) is lower than the World Health Organization’s (110 mg/dL).
Therefore, according to the World Health Organization’s criterion, my fasting blood glucose is still within the normal range. However, the fasting glucose level is right on the lower limit of the ADA’s range for diagnosing impaired fasting glucose.
Glucose Tolerance
Without a 2-hour oral glucose tolerance test, it is impossible to tell if I have impaired glucose tolerance.
Hemoglobin A1c (HbA1c)
MyHbA1c was within the laboratory’s normal range.
Conclusion
Based on my borderline fasting plasma glucose level (5.6 mmol/L, or 100 mg/dL) and following the American Diabetes Association’s diagnostic criteria, I am “prediabetic” and, therefore, at higher risk of developing diabetes mellitus.
However, it seems that intensifying the lifestyle interventions I have used in the past few months will be excessive and may dramatically impact my quality of life. Therefore, I am pushing on with my existing diet and exercise routine to improve my fasting plasma glucose level.